Cardiff Open: Mon-Fri 9:00am-5:30pm (Sat 9am-4pm)
Singleton Open: Mon-Fri 9:00am-5:30pm (Sat Closed)
Fletcher Open: Mon-Fri 9:00am-5:30pm (Sat 9am-1pm)
Mayfield Open: Mon-Fri 9:00am-5:30pm (Sat Closed)
Cardiff : (02) 4954 7722
Singleton : (02) 6572 2526
Fletcher : (02) 4953 8614
Mayfield : (02) 4023 3885Laser Clinic
Laser Dental Treatments
What is Dental Laser?
A Dental Laser is an instrument that produces a narrow intense beam of light energy. When this light beam comes in to contact with tissue, it causes a reaction of cutting or vaporising to shape or remove.
Below is the Laser Equipment Used in Our Surgeries:
“Waterlase”

WaterLase Dentistry
WaterLase dentistry is one of the most advanced dental treatments today. WaterLase uses a patented technology that combines focused light energy with a stream of water for a highly precise, exceptionally gentle dental experience. WaterLase allows your dentist to perform a wide range of procedures with benefits including:
- Faster healing time and less trauma to teeth and gums.
- Less anesthetic for most procedures.
- Treating dental needs in more than one part of the mouth in one visit.
- Making dental care a more relaxing experience for you.
What Can WaterLase Dentistry Do?
We may use WaterLase dentistry laser to treat your gums or other soft tissue in your mouth to:
IMPROVE YOUR SMILE Laser Gingivectomy / Laser Gum Sterilisation
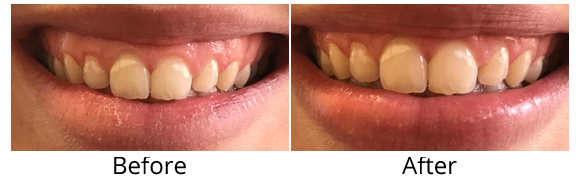
We may suggest contouring or shaping your gums using WaterLase dentistry to improve the appearance of your smile – safely removing excess gum tissue that may give you a “gummy” smile, or make your front teeth appear irregular in size or shape.
Before and after of a Gingivectomy performed by Dr Monika Shah
REMOVE ORAL GROWTHS
Quickly and safely remove growths or excess tissue in your mouth including gum tissue over an unerupted tooth, small “tags” called papilla, and growths called fibromas.
FIX A “TONGUE TIE” OR PREVENT GUM RECESSION – Tongue and Lip tie removal
Connections that restrict the movement of your tongue or cause your gums to recede can be “released” with less post-operative pain. These connections when found on a baby can reduce the movement of the tongue to move freely in the babies’ mouth and cause difficulty for the baby to feed. Releasing these ties can create better function for the baby helping them to feed better and with more comfort
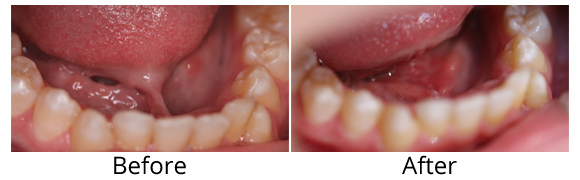
Tongue Tie
Before and After of a laser tongue tie removal preformed by Dr Monika Shah
Lip Tie
TREAT PERIODONTAL DISEASE
We recommend using WaterLase dentistry to remove debris and bacteria between your teeth and gums that can cause bleeding gums, gum recession and even loss of teeth. For moderate to severe gum disease, ask your doctor about REPAIR minimally invasive periodontal treatment.
Exposure of Unerupted Teeth
Impacted teeth are simply those that cannot properly erupt into the mouth. Gums covering the unerupted tooth will be lifted by the laser to expose the hidden tooth underneath.
Operculectomy
Surgical removal of the operculum, a flap of tissue over a partially erupted tooth, particularly the third molar region.
FAQs
It is impossible to make any diagnosis for surgery without taking a full history, carrying out a thorough physical and manual examination conducted by a practitioner with experience treating tongue and lip ties.
A good understanding of the functional issues potentially relating to tongue and/or lip ties is essential and is the reason for the extensive history of symptoms we compile prior to conducting the physical examination. A visual examination is insufficient to determine whether a tongue tie exists, as it is common for a posterior, sub-mucosal tie to be difficult to identify with a visual examination alone. Rather, palpation of the area under the tongue is required by an experienced and appropriately trained practitioner.
The application of anaesthetic will depend on the age of the patient and nature of the procedure. The laser we use has an analgesic effect following application, however this does not usually remove all discomfort and some patients may experience some pain during the brief period of surgery. . For some patients, the taste of the anaesthetic is more disconcerting than the feeling of the laser release. Parents who wish to may also give an age appropriate analgesic to their child about an hour before surgery, although preparations containing ibuprofen (like Nurofen or Advil) and aspirin should not be used.
There is certainly some discomfort associated with any surgery in the oral environment, regardless of the tool. Our laser procedure is customised to provide the best outcomes for each patient depending on their age:
ADULTS YOUTH AND MOST CHILDREN
For adults, youth and most children, the procedure is painless as it is performed under local anaesthetic. A numbing gel is applied prior to the local anaesthetic and can help the discomfort of the needle, once the area is numb the treatment is completed in minimal time.
Pain is very subjective and patients report a variety of pain levels following Laser treatment.
Frenectomy: Laser treatment procedure that is carried out thoroughly (beyond just the membrane of the tie), some pain can be anticipated. To ensure realistic expectations, we anticipate that like the days following any surgery, after a there will naturally be some associated discomfort or pain, mainly during eating. Standard analgesics may be of comfort in the days following surgery.
Gingivectomy: Laser treatment to reduce the level of the gum we would expect some discomfort around the gum area and advice to brush gently in the area with the toothbrush a few days following treatment. Standard analgesics may be of comfort for the first 24 hours.
The type of additional support required is a function of the nature of the challenges being experienced and the age of the patient. Regardless of age, we recommend patients receive manual therapy (chiropractic/osteopathy) in the 24 hours prior to treatment and in the 48 hours subsequent to treatment. Manual therapy from an experienced and appropriately qualified practitioner, increases the suppleness and flexibility of the muscles of the mouth, head and neck, significantly increasing accessibility in the mouth, contributing to positive surgical outcomes. In addition, manual therapy is valuable in teaching new muscle habits and establishing new neural pathways.
In the case of infants undergoing treatment due to problems with breastfeeding, we strongly encourage ongoing lactation support from an appropriately qualified lactation consultant. This is important in helping mother and baby overcome any compensations or habits developed while the tethered oral tissue was still in place
The consultation and surgery at MS Dental is considered a dental procedure and so is currently not covered by Medicare. It may be covered under extras cover with private health insurance. The rebate amount will vary depending on your insurer and level of cover. The codes used are 015 for the consultation and 391 for each laser treatment required.
We advise all patients complete the active wound management protocol stretches every 6 hours for up to 4 weeks post-treatment. We also recommend that patients receive manual therapy from an experiences an appropriately qualified practitioner at least 24-48 hours after surgery. In general, it is best to take things easy in the first couple of days post-surgery and we advise against swimming or other medical procedures (such as immunisations) for seven days after the procedure.
While it is impossible to say for certain whether a tongue or lip tie in a child will lead to specific orofacial issues in later life, tongue ties have been linked to a number of potential issues across the lifespan.
For some time, studies have shown the effects of a “descended tongue posture” and “tongue thrusts” on the development of the jaws, positioning of the teeth, certain breathing dysfunctions (please contact us for details of these publications)
Given the importance of breastfeeding in strengthening the tongue and other mouth and face muscles and the important role of the tongue in encouraging correct tongue posture (where we place our tongue at rest), the inability or ineffectiveness of many tongue tied infants to breastfeed adequately may led to poor tongue positioning. Even after breastfeeding has ceased, the establishment of tongue posture and the patterns of tongue movement may be limited by a tongue restriction.
An example of poor tongue posture is where it sits at the bottom of the mouth, rather than resting on the mid-front part of the hard palate (behind the upper teeth). This positioning along with the pressures placed on the particularly malleable hard tissue of the mouth and face in early childhood caused by incorrect tongue positioning or absence of suitable tongue pressure during breastfeeding can cause many tongue tied infants to develop a high arched or “bubble” palate and ultimately a narrow jaw. This may in turn result in obstruction within the nasal airways and may lead to mouth breathing .
Habitual mouth breathing in turn, alters the development of the mandible (lower jaw) resulting in a chin/jaw that sits relatively recessed in comparison to its optimum position (retrognathia) and an over bite. A narrow jaw has limited space for the eruption of adult sized teeth and may result in dental crowding, resulting in malocclusion (poor bite) which can lead to poor oral hygiene, uneven tooth wear and pain in the temporomandibular joint (where the lower jaw hinges with the skull). These issues often require treatment such as braces. Given the important role nasal breathing plays in humidifying and decontaminating air, persistent mouth breathing may also result in frequent infection of the throat and tonsils and the upper respiratory tract.
Recent experience indicates the pressures created in the muscles of the mouth, head and neck caused by tethered oral tissue and poor tongue posture may also be a cause of poor posture and cervical (neck) and thoracic (upper back) pain.
It is important to re-iterate that a tongue restriction may not necessarily lead to all of these issues. It merely may influence the tongue’s ability to fully affect the development of the mouth and face and depending on many other variables, will contribute its part in affecting the growth and development of the face. Also treatment of a tongue restriction does not guarantee the elimination of all these issues – it is the removal of a postulated contributor to future issues.
Traditionally tongue and lip ties were cut with scissors, however with the advancement of technology laser treatments can now be used to treat these oral restrictions. It is impossible to make any diagnosis for surgery without taking a full history, carrying out a thorough physical and manual examination conducted by a practitioner with experience treating tongue and lip ties.
A good understanding of the functional issues potentially relating to tongue and/or lip ties is essential and is the reason for the extensive history of symptoms we compile prior to conducting the physical examination. A visual examination is insufficient to determine whether a tongue tie exists, as it is common for a posterior, sub-mucosal tie to be difficult to identify with a visual examination alone. Rather, palpation of the area under the tongue is required by an experienced and appropriately trained practitioner.
For patients who have had a tongue or lip tie treated, we advise all patients complete the active wound management protocol stretches every 6 hours for up to 4 weeks post-treatment. We also recommend that patients receive manual therapy from an experiences an appropriately qualified practitioner at least 24-48 hours after surgery. In general, it is best to take things easy in the first couple of days post-surgery and we advise against swimming or other medical procedures for seven days after the procedure.
For patients who have had laser treatment such as gingivectomy we recommend to take things easy for the next day or two after the surgery and to keep the area clean by gently brushing with the toothbrush. Gentle salt water rinses can also be helpful in the healing process of the gum area.















